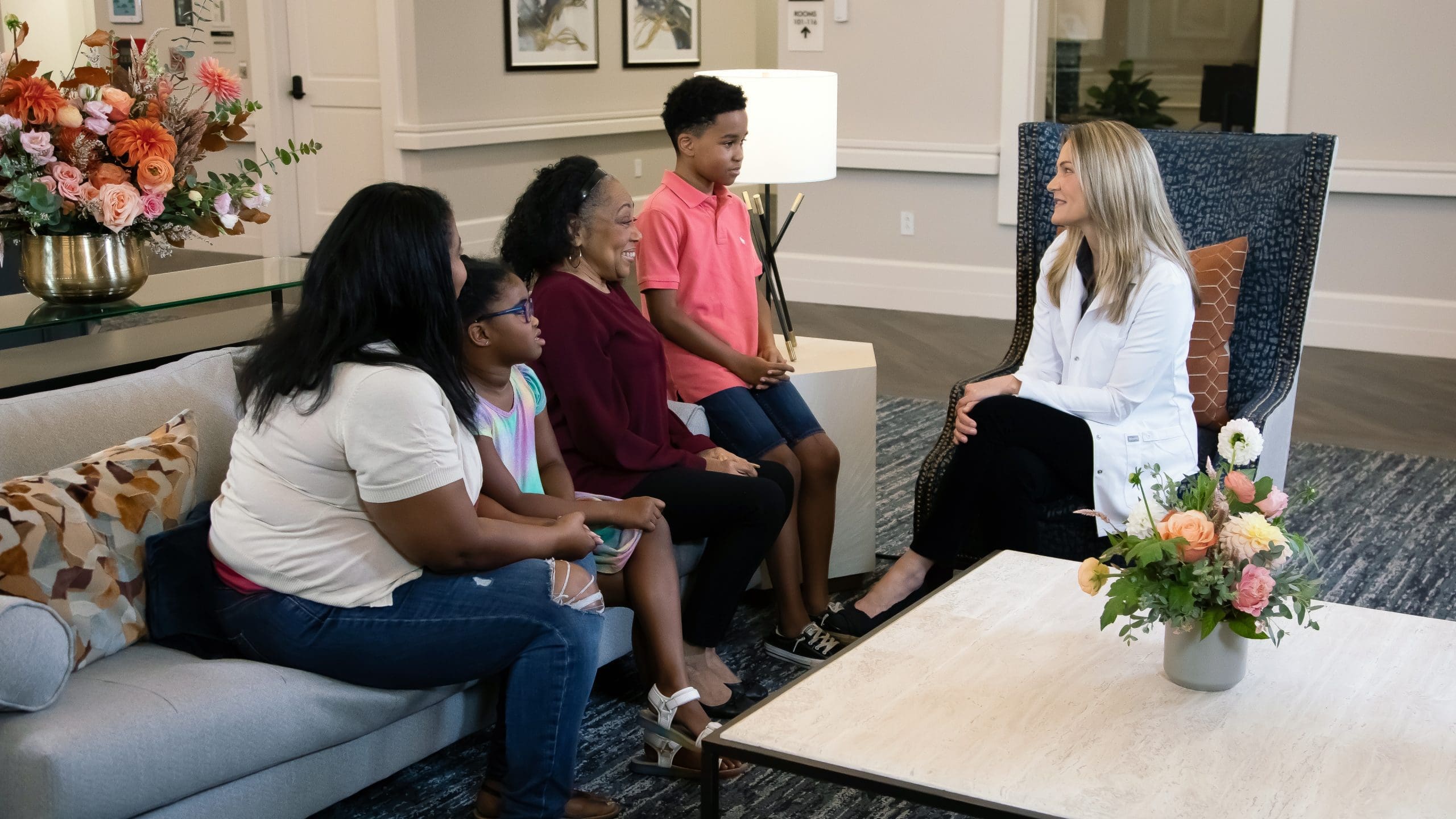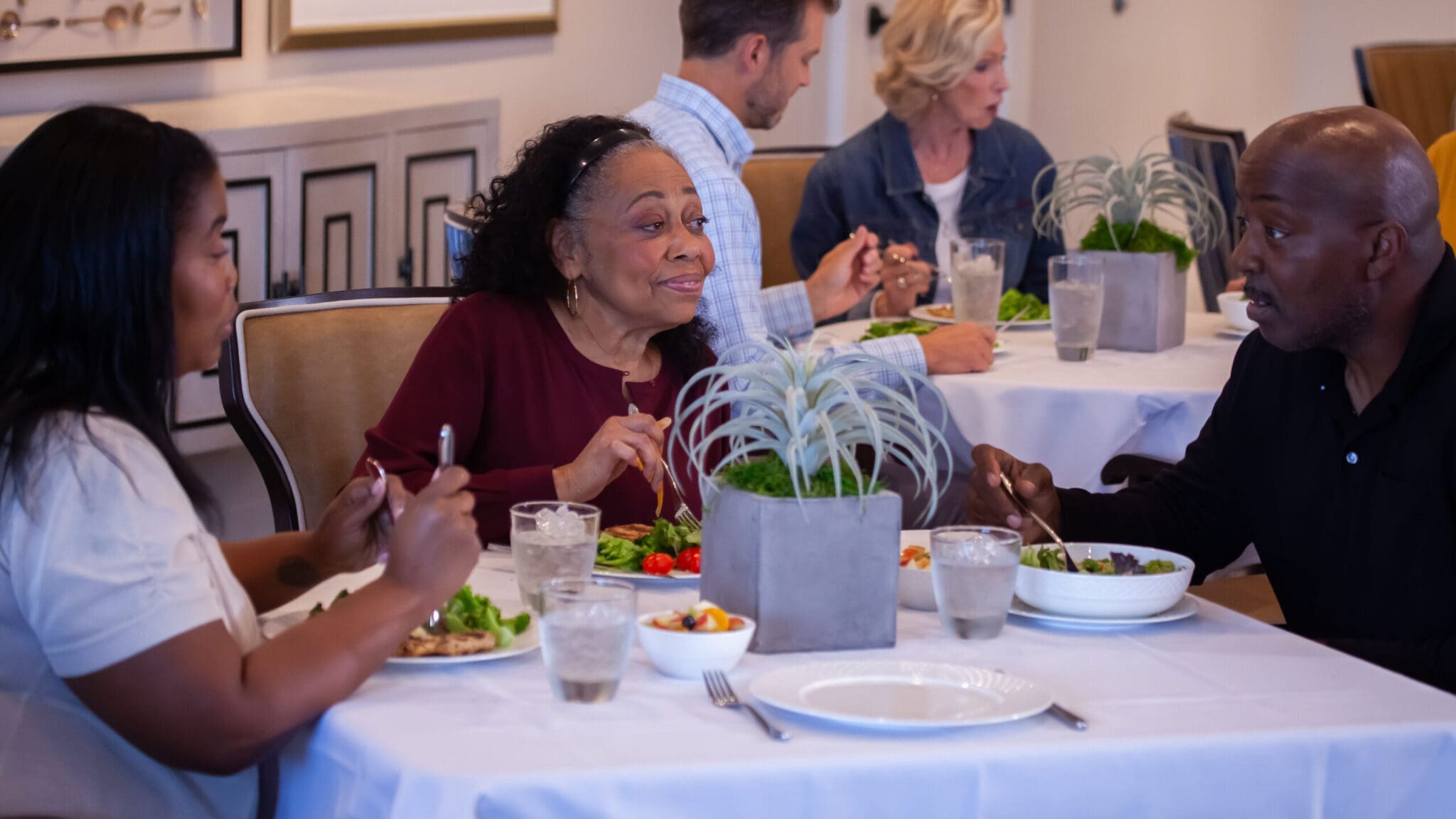Aspen Transitional Rehabilitation
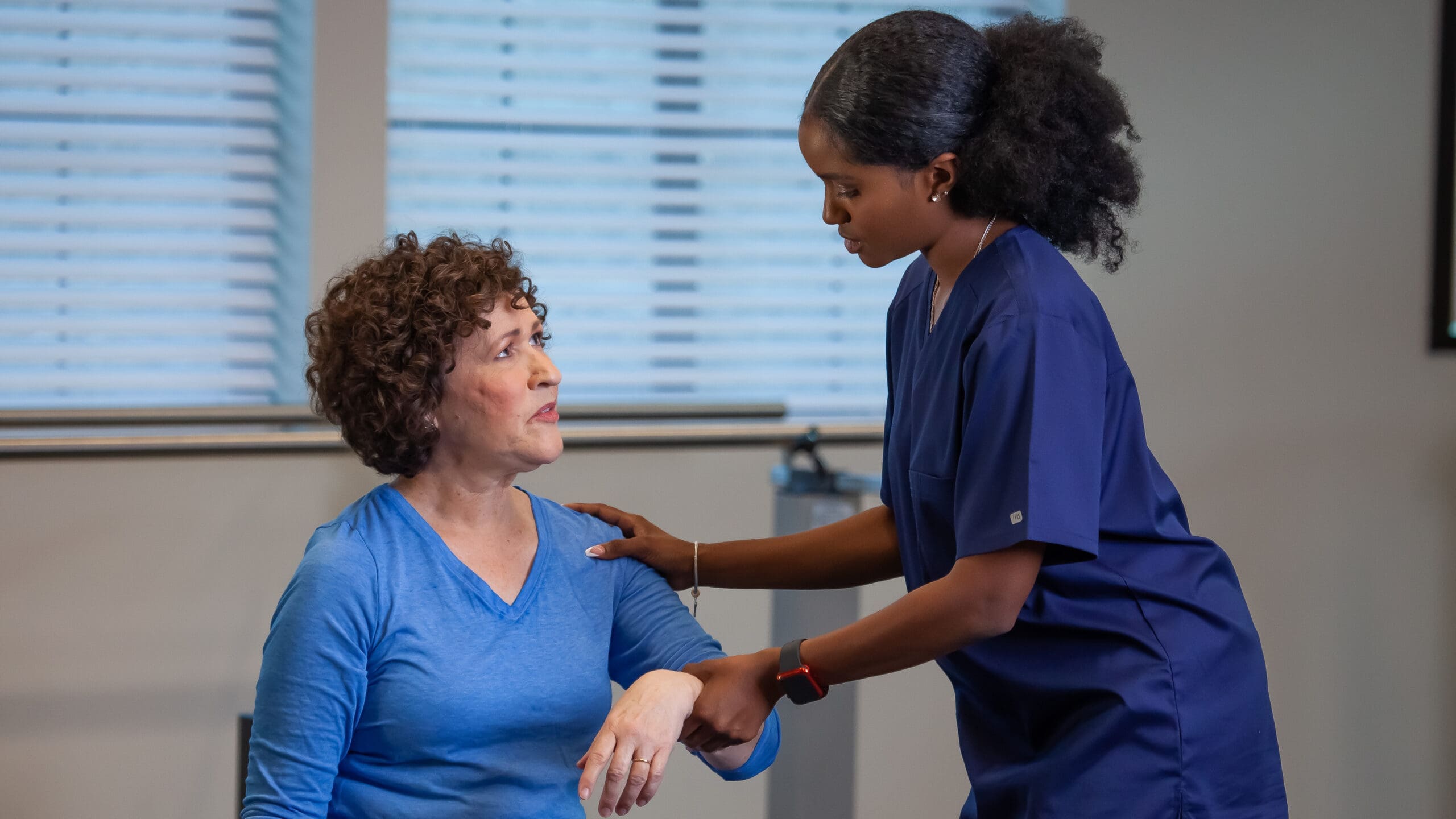
Aspen Transitional Rehabilitation maintains a level of elegance and professionalism for its residents, promoting mutual respect and trust. The upscale nursing home aims to reinvent the meaning of skilled nursing and rehabilitation for seniors through the exceptional level of care delivered by their patient-friendly staff to offer the best care possible for their residents.
The nursing homes provide state-of-the-art features that cater to short-term or long-term residents; they also are guaranteed to feel comfortable and know that they belong in a home that offers 24-hour nursing care with inpatient and outpatient care in a resort-like community with the utmost level of hospitality.
Types of Care at Aspen Transitional Rehabilitation
About this community
Staffing
Key information about the people who lead and staff this community.
Quality of care over time
These measures show how residents usually do over time at this home, based on health outcomes and preventive care.
Short-stay resident measures
Places of interest near Aspen Transitional Rehabilitation
3.7 miles from city center
Estimated distance in miles from Meridian's city center to Aspen Transitional Rehabilitation's address, calculated via Google Maps.
— 1.16 miles to nearest hospital (St. Luke's Meridian Medical Center)
Calculate Travel Distance to Aspen Transitional Rehabilitation
Add your location
Financial Assistance for
Nursing Home in Idaho
Aspen Transitional Rehabilitation is located in Meridian, Idaho.
Here are the financial assistance programs available to residents in Idaho.
Frequently Asked Questions about Aspen Transitional Rehabilitation
What neighborhood is Aspen Transitional Rehabilitation in?
Aspen Transitional Rehabilitation is in the El Dorado Business Campus neighborhood of Meridian.
Is Aspen Transitional Rehabilitation in a walkable area?
Aspen Transitional Rehabilitation has a walk score of 44. Somewhat walkable. A few nearby services may be reachable on foot, but most trips require transportation.
Are there photos of Aspen Transitional Rehabilitation?
Yes — there are 21 photos of Aspen Transitional Rehabilitation in the photo gallery on this page.
What is the phone number of Aspen Transitional Rehabilitation?
(208) 401-9100 will put you in contact with the team at Aspen Transitional Rehabilitation.
Is Aspen Transitional Rehabilitation Medicare or Medicaid certified?
Yes — Aspen Transitional Rehabilitation is a CMS-certified provider of Medicare and Medicaid.
Guides for Better Senior Living
Care Cost Calculator: See Prices in Your Area
Nursing Home Data Explorer
Don’t Wait Too Long: 7 Red Flag Signs Your Parent Needs Assisted Living Now
The True Cost of Assisted Living in 2025 – And How Families Are Paying For It
Understanding Senior Living Costs: Pricing Models, Discounts & Financial Assistance
Contact Us

Write a review for Aspen Transitional Rehabilitation
Rate your overall experience with this community
Thank you for your interest!
Our team will be in touch shortly to help with next steps.
Need Help?
Let us help you or a loved one find the perfect senior home.