Valley Eldercare Center
Situated in Grand Forks, North Dakota, Valley Eldercare Center is a retirement community that offers a perfect balance of independence and care. Ideal for couples, siblings, and friends, this community provides multiple services tailored to individual needs, allowing loved ones to stay close to each other while receiving personalized attention.
Discover the freedom of apartment living and the convenience of being near healthcare specialists at Valley Senior Living on 42nd. Immerse yourself in a friendly and social atmosphere, fostering new friendships and connections with neighbors. Embrace a vibrant retirement lifestyle in the heart of Grand Forks at Valley Senior Living.
About this community
Staffing
Key information about the people who lead and staff this community.
Inspection History
In North Dakota, the Department of Health and Human Services, Health Facilities Division is the agency authorized to perform unannounced inspections and issue official health quality reports.
Inspection Scorecard
 This scorecard compares key inspection, citation, and complaint metrics at this facility against the North Dakota state average. Metrics rated ≥15% worse than average are highlighted in red; those ≥15% better are highlighted in green.
This scorecard compares key inspection, citation, and complaint metrics at this facility against the North Dakota state average. Metrics rated ≥15% worse than average are highlighted in red; those ≥15% better are highlighted in green.
Since 2023 vs. North Dakota state average
• Total deficiencies (5% above)
• Deficiencies per year (5% above) 0 Better No metrics in this bucket.
Deficiencies
|
This Facility | ND Average | vs. ND Avg |
|---|---|---|---|
|
Total deficiencies
|
23 | 22 | This facility has 5% more total deficiencies than a typical North Dakota nursing home (23 vs. ND avg 22).↑ 5% worse |
|
Deficiencies per year
|
7.7 | 7.3 | This facility has 5% more deficiencies per year than a typical North Dakota nursing home (7.7 vs. ND avg 7.3).↑ 5% worse |
Inspection Reports Summary
 An editor-reviewed summary of the themes and findings across this facility's recent inspection reports.
An editor-reviewed summary of the themes and findings across this facility's recent inspection reports.
- June 19, 2025 annual inspection found 3 deficiencies involving MDS coding, fall prevention, and infection control, with no immediate jeopardy or fines reported.
- August 19, 2025 complaint investigation substantiated sexual abuse between residents, citing failure to protect residents from abuse and requiring monitoring and care plan updates.
- May 16, 2024 annual inspection identified 7 deficiencies including fall prevention failures causing fractures, inadequate supervision, pressure ulcer care, and infection control lapses.
Quality of care over time
These measures show how residents usually do over time at this home, based on health outcomes and preventive care.
Long-stay resident measures
Short-stay resident measures
What does this home offer?
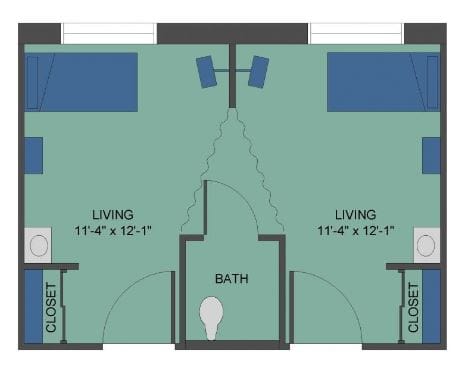
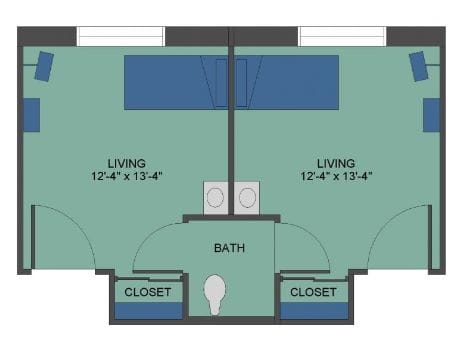
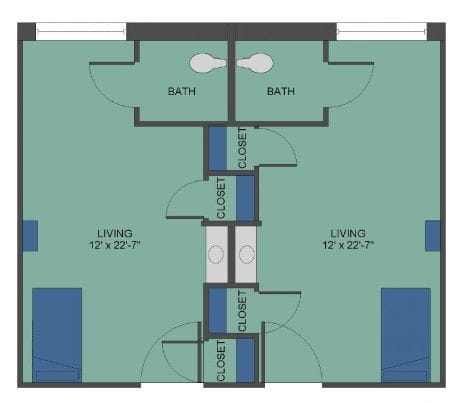
Housing Options: Private Rooms / Semi-Private Rooms
Building Type: Single-story
Transportation Services
Fitness and Recreation
Places of interest near Valley Eldercare Center
3.0 miles from city center
Estimated distance in miles from Grand Forks's city center to Valley Eldercare Center's address, calculated via Google Maps.
— 0.04 miles to nearest hospital (Altru's Prosthetic & Orthotic Department)
Calculate Travel Distance to Valley Eldercare Center
Add your location
Financial Assistance for
Nursing Home in North Dakota
Valley Eldercare Center is located in Grand Forks, North Dakota.
Here are the financial assistance programs available to residents in North Dakota.
Frequently Asked Questions about Valley Eldercare Center
Is Valley Eldercare Center in a walkable area?
Valley Eldercare Center has a walk score of 53. Moderately walkable. Some errands can be accomplished on foot, with a mix of nearby amenities.
Are there photos of Valley Eldercare Center?
Yes — there are 5 photos of Valley Eldercare Center in the photo gallery on this page.
What is the phone number of Valley Eldercare Center?
(701) 787-7900 will put you in contact with the team at Valley Eldercare Center.
Is Valley Eldercare Center Medicare or Medicaid certified?
Valley Eldercare Center is not currently listed as a CMS-certified provider of Medicare or Medicaid.
Guides for Better Senior Living
Care Cost Calculator: See Prices in Your Area
Nursing Home Data Explorer
Don’t Wait Too Long: 7 Red Flag Signs Your Parent Needs Assisted Living Now
The True Cost of Assisted Living in 2025 – And How Families Are Paying For It
Understanding Senior Living Costs: Pricing Models, Discounts & Financial Assistance
Contact Us

Write a review for Valley Eldercare Center
Rate your overall experience with this community
Thank you for your interest!
Our team will be in touch shortly to help with next steps.
Need Help?
Let us help you or a loved one find the perfect senior home.