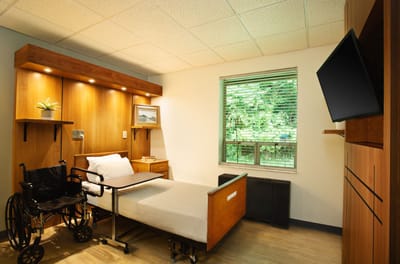
South Roanoke Nursing and Rehabilitation
Providing top-tier care since 1964, South Roanoke Nursing and Rehabilitation located in the serene community of Franklin Road, South West Roanoke, VA, focuses on rehabilitation, skilled care, long-term care, and respite. The community promises a comfortable and safe residence while receiving the utmost attention for their needs. Spend a relaxing time within the beautiful grounds with heartwarming individuals. South Roanoke Nursing and Rehabilitation is dedicated to giving seniors a warm and welcoming environment during their healing journey.
South Roanoke Nursing and Rehabilitation takes pride in a team of reliable and highly skilled professionals, who deliver exceptional care and support. With its stunning amenities and peaceful surroundings, seniors enjoy leisure while maintaining their well-being. The community is a safe place for seniors to thrive and reach their full potential.
How BBB ratings work
About this community
Staffing
Key information about the people who lead and staff this community.
Quality of care over time
These measures show how residents usually do over time at this home, based on health outcomes and preventive care.
Long-stay resident measures
Short-stay resident measures
Finances and operations
What does this home offer?
Housing Options: Private Rooms
Building Type: Single-story
Fitness and Recreation
Places of interest near South Roanoke Nursing and Rehabilitation
3.4 miles from city center
Estimated distance in miles from Roanoke's city center to South Roanoke Nursing and Rehabilitation's address, calculated via Google Maps.
— 1.86 miles to nearest hospital (Carilion Clinic Aortic Center - Roanoke)
Calculate Travel Distance to South Roanoke Nursing and Rehabilitation
Add your location
Financial Assistance for
Nursing Home in Virginia
South Roanoke Nursing and Rehabilitation is located in Roanoke, Virginia.
Here are the financial assistance programs available to residents in Virginia.
Compare Nursing Home around Roanoke
The information below is reported by the Virginia Department of Social Services and Department of Health.
| Our Lady of the Valley |
NH Nursing Home Licensed facility providing 24/7 skilled nursing care for residents with complex, ongoing medical needs. Staffed by RNs, LPNs, and CNAs. Inspected and star-rated annually by CMS. Accepts Medicare (short-term rehab) and Medicaid (long-term care).
AL Assisted Living A licensed, long-term care setting for seniors or individuals with disabilities who need help with daily activities — like bathing, dressing, and medication management — but not 24-hour skilled nursing. Offers housing, meals, and around-the-clock support while aiming to maximize resident independence.
IL Independent Living Lifestyle-focused communities for older adults offering dining, activities, and transportation with minimal personal care. Best for active, independent seniors who want community without medical support.
MC Memory Care Secured, specialized care for people living with Alzheimer's or dementia. Staff trained in cognitive impairment, with higher staff-to-resident ratios and an environment designed to reduce confusion and wandering risk. | Roanoke (Gainsboro) | 127
Facility
127
VA AVG
98
Rank
#82 / 371 | 87.4% | +2% | 3.79 | -42% | +1% | $0 | 14 | 4.7 | - | 111 | A+ |
68
Facility
68
VA AVG
44
Rank
#74 / 449 | David Rawlings | $17.2M | $8.2M | 47.6% | 495357 | ||||
| Pheasant Ridge Nursing and Rehab Center |
NH Nursing Home Licensed facility providing 24/7 skilled nursing care for residents with complex, ongoing medical needs. Staffed by RNs, LPNs, and CNAs. Inspected and star-rated annually by CMS. Accepts Medicare (short-term rehab) and Medicaid (long-term care).
AL Assisted Living A licensed, long-term care setting for seniors or individuals with disabilities who need help with daily activities — like bathing, dressing, and medication management — but not 24-hour skilled nursing. Offers housing, meals, and around-the-clock support while aiming to maximize resident independence.
IL Independent Living Lifestyle-focused communities for older adults offering dining, activities, and transportation with minimal personal care. Best for active, independent seniors who want community without medical support.
MC Memory Care Secured, specialized care for people living with Alzheimer's or dementia. Staff trained in cognitive impairment, with higher staff-to-resident ratios and an environment designed to reduce confusion and wandering risk. | Roanoke (Southern Hills) | 101
Facility
101
VA AVG
98
Rank
#144 / 371 | - | - | 3.56 | +4% | -5% | $45.3k | 25 | 6.3 | 1 | 19 | A+ |
15
Facility
15
VA AVG
44
Rank
#385 / 449 | Victor Bell | $14.5M | $5.1M | 35.5% | 495325 |
Frequently Asked Questions about South Roanoke Nursing and Rehabilitation
What neighborhood is South Roanoke Nursing and Rehabilitation in?
South Roanoke Nursing and Rehabilitation is in the Edgehill neighborhood of Roanoke.
Is South Roanoke Nursing and Rehabilitation in a walkable area?
South Roanoke Nursing and Rehabilitation has a walk score of 45. Somewhat walkable. A few nearby services may be reachable on foot, but most trips require transportation.
Are there photos of South Roanoke Nursing and Rehabilitation?
Yes — there are 5 photos of South Roanoke Nursing and Rehabilitation in the photo gallery on this page.
What is the phone number of South Roanoke Nursing and Rehabilitation?
(540) 344-4325 will put you in contact with the team at South Roanoke Nursing and Rehabilitation.
Is South Roanoke Nursing and Rehabilitation Medicare or Medicaid certified?
Yes — South Roanoke Nursing and Rehabilitation is a CMS-certified provider of Medicare and Medicaid.
Guides for Better Senior Living
Care Cost Calculator: See Prices in Your Area
Nursing Home Data Explorer
Don’t Wait Too Long: 7 Red Flag Signs Your Parent Needs Assisted Living Now
The True Cost of Assisted Living in 2025 – And How Families Are Paying For It
Understanding Senior Living Costs: Pricing Models, Discounts & Financial Assistance
Contact Us

Write a review for South Roanoke Nursing and Rehabilitation
Rate your overall experience with this community
Thank you for your interest!
Our team will be in touch shortly to help with next steps.
Need Help?
Let us help you or a loved one find the perfect senior home.